Bariatric Surgery
Medical Tourism
Gastric Sleeve (Sleeve Gastrectomy)
R3 Medical Tourism | Elite Bariatric Care in Tijuana, Mexico
What Is a Gastric Sleeve?
The gastric sleeve—formally known as a sleeve gastrectomy or vertical sleeve gastrectomy (VSG)—is the most commonly performed bariatric surgery in the world, accounting for more than half of all weight-loss procedures globally. The operation permanently removes approximately 75 to 80 percent of the stomach, transforming it from a large, J-shaped organ into a narrow, banana-shaped tube (or “sleeve”) with a capacity of approximately 60 to 150 milliliters—roughly the size of a small banana. The portion of the stomach removed includes the fundus, which is the area that produces most of the hunger-stimulating hormone ghrelin, giving the sleeve gastrectomy a powerful dual mechanism of action.
Unlike older restrictive procedures, the gastric sleeve works through two complementary pathways. First, the dramatically reduced stomach volume limits the amount of food that can be consumed at a single sitting, creating a feeling of fullness and satisfaction with far smaller portions than before surgery. Second, the removal of the ghrelin-producing fundus substantially reduces hunger hormone levels, meaning patients not only feel full faster but are also significantly less hungry throughout the day. This hormonal effect is one of the key reasons sleeve gastrectomy produces more sustained weight loss than purely restrictive procedures such as the adjustable gastric band.
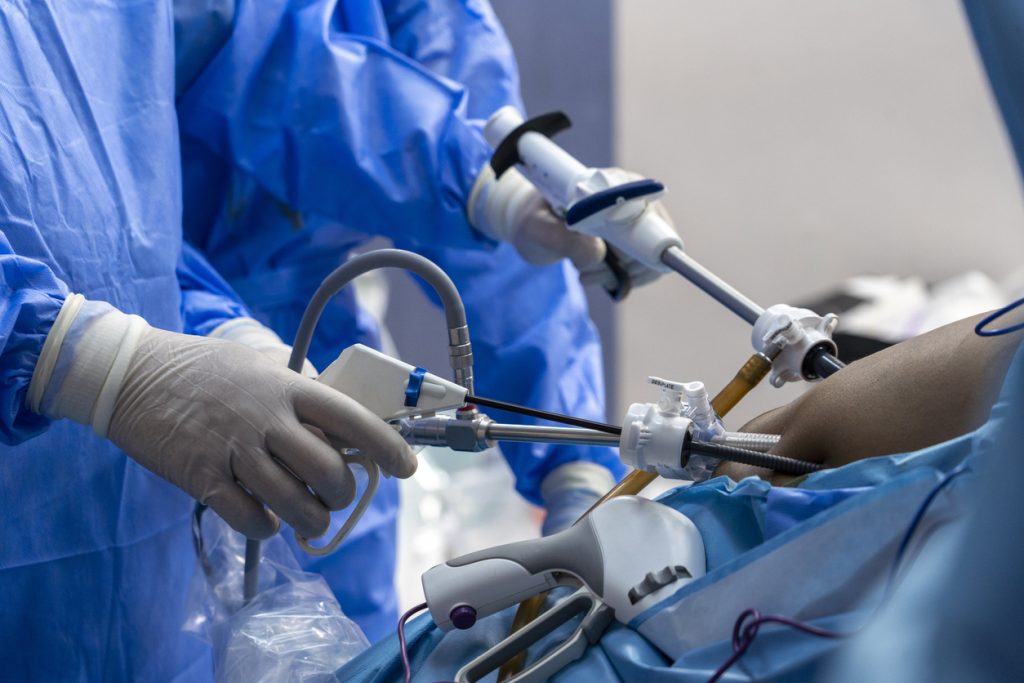
The gastric sleeve is performed laparoscopically through small abdominal incisions, making it a minimally invasive procedure with a rapid recovery. It does not involve any rerouting of the intestines, so the normal digestive pathway is preserved—nutrients are absorbed along the entire length of the small intestine, and the risk of nutritional deficiencies, while present, is lower than with malabsorptive procedures such as gastric bypass. The sleeve is a permanent, non-reversible procedure, and the removed stomach tissue cannot be restored.
Who Is a Gastric Sleeve For?
Sleeve gastrectomy is appropriate for adults with a body mass index (BMI) of 40 or higher (Class III obesity), or adults with a BMI of 35 to 39.9 (Class II obesity) who also have at least one serious obesity-related health condition—such as type 2 diabetes, hypertension, obstructive sleep apnea, non-alcoholic fatty liver disease, or osteoarthritis of weight-bearing joints. In recent years, evidence has expanded to support sleeve gastrectomy for patients with a BMI of 30 to 34.9 who have poorly controlled type 2 diabetes or metabolic syndrome, with some guidelines and professional societies now endorsing surgical intervention at this lower BMI threshold.
The ideal candidate has made sustained but unsuccessful attempts to lose weight through non-surgical means—including structured dietary programs, physical activity, and pharmacological therapy—and understands that bariatric surgery is a tool that requires lifelong dietary and lifestyle commitment to achieve and maintain optimal results. Patients must be medically cleared for surgery, with no untreated serious psychiatric conditions that would impair their ability to follow post-operative guidelines, and must understand the permanence of the procedure.
The sleeve is often the preferred procedure for patients who are higher surgical risk—including the elderly, those with complex medical comorbidities, or super-obese patients (BMI >50) for whom it may be used as the first stage of a two-step approach before a subsequent revision to gastric bypass or duodenal switch. It is also a suitable choice for patients who wish to avoid the intestinal rerouting of gastric bypass or who have concerns about long-term malabsorption.
Frequently Asked Questions
It is a long established fact that a reader will be distracted by the readable content of a page when looking at its layout. The point of using Lorem Ipsum is that it has a more-or-less normal distribution of letters, as opposed to using..
Why Get a Gastric Sleeve in Tijuana, Mexico?
In the United States, sleeve gastrectomy costs between $15,000 and $30,000 at most accredited bariatric centers, and insurance coverage—while expanding—remains inconsistent, requiring extensive documentation of prior failed weight-loss attempts, supervised diet programs, and lengthy pre-authorization processes that can delay surgery by 6 to 12 months or more. For patients without insurance coverage or with high out-of-pocket costs, these barriers make surgery financially and logistically inaccessible.
Tijuana, Mexico, is the most popular destination in the world for bariatric surgery medical tourism, with an estimated 40,000 to 60,000 patients traveling to Tijuana annually for weight-loss procedures. R3 Medical Tourism’s network of elite bariatric surgeons in Tijuana offers sleeve gastrectomy at a fraction of U.S. costs—typically $4,000 to $7,000 all-inclusive—performed by board-certified bariatric surgeons with thousands of procedures in their experience. These surgeons are fellowship-trained in minimally invasive bariatric surgery, operate in fully accredited, Joint Commission International-level facilities, and follow evidence-based perioperative protocols aligned with the American Society for Metabolic and Bariatric Surgery (ASMBS) guidelines.
The geographic proximity of Tijuana to the United States—just across the border from San Diego—makes it highly accessible to patients from California, Arizona, Nevada, and beyond. R3 Medical Tourism coordinates all aspects of the surgical journey, including pre-operative evaluation, surgical consultation, procedure, hospital stay, and post-operative follow-up, ensuring patients receive comprehensive, professionally managed care from start to finish.
How Is a Gastric Sleeve Performed?
Sleeve gastrectomy is performed laparoscopically under general anesthesia. The surgeon makes three to five small incisions (5 to 12 mm) in the abdomen through which a laparoscope and surgical instruments are introduced. The abdomen is insufflated with carbon dioxide gas to create a working space. The greater curvature of the stomach is fully mobilized by dividing the short gastric vessels and the gastrocolic ligament, freeing the stomach from its lateral attachments.
A sizing bougie—a calibrated tube typically 32 to 40 French in diameter—is passed orally by the anesthesiologist into the stomach to guide the resection and ensure a consistent sleeve size. Using a laparoscopic stapler, the surgeon sequentially fires staple lines along the greater curvature from the antrum (the lower portion of the stomach, approximately 2 to 6 cm from the pylorus) to the angle of His at the gastroesophageal junction, removing the fundus and most of the body of the stomach. The excised stomach is removed through one of the port sites. A leak test—performed by insufflating the sleeve with air or methylene blue dye—confirms staple line integrity before closing.
The procedure takes approximately 45 to 90 minutes. Most patients are admitted to the hospital for one to two nights and are discharged on a liquid diet that is advanced gradually over four to six weeks: clear liquids for the first two weeks, full liquids for weeks three and four, pureed foods for weeks five and six, and then a progression to soft and regular foods. Full dietary freedom—with appropriate portion control—is typically achieved by three to six months post-surgery.
Outcomes and What the Data Shows
Sleeve gastrectomy produces reliable, substantial, and durable weight loss with an excellent safety profile. Large-scale published series and meta-analyses consistently report mean excess weight loss (EWL) of 60 to 70 percent at one year and total body weight loss (%TBWL) of 25 to 30 percent. Long-term follow-up data—now extending to 5 to 10 years—demonstrate maintained %TBWL of 20 to 25 percent in the majority of patients, with some weight regain expected at 3 to 5 years that is generally modest compared to non-surgical weight loss interventions.
The metabolic benefits of sleeve gastrectomy are profound. Type 2 diabetes remission—defined as normal blood sugar without medication—is achieved in approximately 60 to 70 percent of patients, with significant improvement in glycemic control in the remaining diabetic patients. Hypertension resolves or improves in 65 to 75 percent of patients, obstructive sleep apnea resolves in approximately 85 percent, and dyslipidemia improves in over 70 percent. These metabolic improvements are often apparent within weeks of surgery—before substantial weight loss has occurred—reflecting the hormonal rather than purely mechanical effects of the procedure.
The 30-day mortality rate for laparoscopic sleeve gastrectomy at experienced centers is approximately 0.1 to 0.3 percent—lower than the mortality for gallbladder removal—and the major complication rate is approximately 2 to 3 percent, with staple line leak (occurring in approximately 1 to 2 percent of cases) being the most serious potential complication. At R3 Medical Tourism’s partner centers in Tijuana, these outcomes benchmarks are routinely met and monitored, with leak rates and complication rates tracked against international quality standards.
Ready to take the next step toward lasting weight loss and better health? Contact R3 Medical Tourism today to connect with an elite bariatric specialist in Tijuana, Mexico. World-class surgical expertise, proven outcomes, and significant cost savings are within reach.
Other Available Bariatric Surgery
It is a long established fact that a reader will be distracted by the readable content of a page when looking at its layout. The point of using Lorem Ipsum is that it has a more-or-less normal distribution of letters, as opposed to using..

Roux-En-Y Gastric
Bypass
It is a long established fact that a reader will be distracted by the readable content

Adjustable Gastric Banding (lap band)
It is a long established fact that a reader will be distracted by the readable content

Duodenal Switch
It is a long established fact that a reader will be distracted by the readable content of a page when looking at its layout

Single Anastomosis Duodeno-Ileal Bypass (SADI)
It is a long established fact that a reader will be distracted by the readable content

Mini Gastric Bypass
It is a long established fact that a reader will be distracted by the readable content of a page when looking at its layout
Gastric Balloon
(Intragastric Balloon)
It is a long established fact that a reader will be distracted by the readable content
Endoscopic Sleeve Gastroplasty
It is a long established fact that a reader will be distracted by the readable content

Revision Bariatric
Surgery
It is a long established fact that a reader will be distracted by the readable content
Post-Bariatric
Body Contouring
It is a long established fact that a reader will be distracted by the readable content
Schedule your free consultation at 80+ Centers worldwide
Success Stories
It is a long established fact that a reader will be distracted by the readable content of a page when looking at its layout. The point of using Lorem Ipsum is that it has a more-or-less normal distribution of letters, as opposed to using..
Looking Forward To Hearing From You !
Our Location
1521 E Windsor #6 Glendale CA 91205 US
Email Address
info@r3medicaltourism.com
Call Us Now
123 456 7890
